|
OmniCare ills haunt health care
Debt grew under state's watch

by Sarah A. Webster / The Detroit News
/ July 14, 2002

DETROIT -- Doctors and hospitals want
an investigation into how OmniCare Health Plan went more than
$100 million in debt to them while state regulators were
supervising the insolvent Detroit managed-care company.
The Detroit Medical Center, which owns seven hospitals and
clinics throughout southeast Michigan, and other health care
companies on Friday asked Ingham County Circuit Judge James
Giddings for an independent counsel to investigate mismanagement
and potential fraud in the case. He's considering the request.
"I firmly believe OmniCare's financial problems are due to
mismanagement on a scale that rivals the Enron scandal," said
Dr. Daniel Michael, chief of neurosurgery at Detroit Receiving
Hospital.
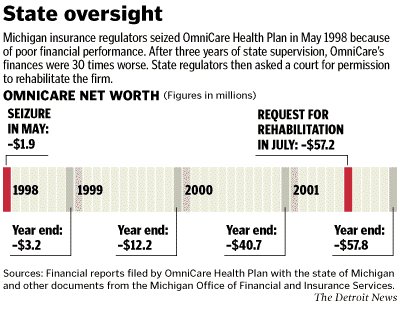
The state's 10th largest health maintenance organization,
OmniCare was seized by the Michigan Office of Financial and
Insurance Services in May 1998. But under state supervision, the
nonprofit company's net worth -- its assets minus liabilities --
went from negative $1.9 million to negative $57.2 million in
July 2001.
The financial mess has left unpaid bills for about 500
physicians, hospitals and nursing agencies, who are under court
order to continue providing services to OmniCare members. It's
putting a financial strain on health care companies and hurting
the quality of patient care, health officials said.
Judge Giddings is considering approving a plan by state
insurance officials to reorganize the debt-ridden company. But
health care providers question how state officials can turn
around the HMO when it deteriorated under its watch.
"The administration in Lansing has to bear some of the blame
for the way this company has been allowed to operate," said Dr.
Lonnie Joe, president of the Detroit Medical Society, which
represents more than 400 black doctors in southeast Michigan.
Michigan Insurance Commissioner Frank Fitzgerald, who took
office in 1999, said the state has appropriately monitored the
company and that OmniCare deserves to be revived.
"It's a proud company that can and should continue operating
into the future," he said.
But health care providers say the state has a conflict of
interest. The majority of OmniCare's debt stems from its state
contract to manage the health of as many as 66,636 Medicaid
clients. The HMO also has about 30,000 commercial members.
Michigan taxpayers have paid OmniCare $452 million since 1998
for that Medicaid service.
"Where was the money going?" Michael asked.
Criticize management
Doctors and hospitals are also criticizing the management of
United American
Healthcare Corp., which has managed OmniCare since 1985, for
the HMO's problems in recent years.
In court documents, the DMC and St. John Health System accuse
United American of fraudulently transferring money to OmniCare
without providing a reasonable service in return. Fitzgerald has
recommended terminating the relationship between OmniCare and
United American.
But Gregory Moses, United American's chief executive, said
the state insurance department approved every action taken at
OmniCare since 1998.
"The state was in charge," Moses said. "They always
controlled the checkbook."
Hospitals and doctors have written to federal officials with
the U.S. Centers for Medicare and Medicaid and talked with
legislators, seeking an investigation into the management and
oversight of the HMO.
While the financial situation crumbled at OmniCare, so did
the quality of patient care.
The HMO's rating with the National Committee for Quality
Assurance dropped from "commendable" to "provisional," or one
notch from losing accreditation. OmniCare did not meet basic
requirements for providing access to needed care, good customer
service or quality preventive health programs.
Patricia Luker of Royal Oak said OmniCare caused her
"personal torment."
Her daughter, Jessica Baccus, was using Medicaid because she
had a rare brain disorder, and the state later put her into
OmniCare. Medicaid patients can select and change their HMO
during enrollment periods, but the state also can put patients
into an HMO.
Once in the HMO, the family had trouble getting bills paid
and finding a doctor. Jessica died Sept. 10, 1999, at the age of
24, and the problems made Luker an advocate for a federal
Patient Bill of Rights.
"They didn't provide us with any physician in their catalog
in the tri-county area that would accept Jessica," she said.
In hundreds of pages of documents filed in Ingham and Oakland
county courts, a picture emerges of how OmniCare sunk into
insolvency. Formerly known as Michigan HMO, OmniCare was one of
the country's first HMOs, serving the state since 1973.
But hospitals and doctors cite conflicts of interest in
recent years -- between the state of Michigan, OmniCare and
United American -- that may have contributed to the HMO's
troubles.
Seized in 1998
Michigan insurance regulators first seized OmniCare's assets
under a sealed court order in 1998 for failing to pay its bills
on time, understating its debts and being insolvent. The state
kept United American on to manage the company, and they put
together a turnaround plan that year.
But OmniCare, still under state watch, continued to not pay
bills on time and understate its debts, insurance officials
said. It also did not prepare budgets or balance its checkbook
in recent years, the state says.
Southfield Dr. Dhia L. Yousif said OmniCare's books don't
reveal $12,418 owed to him.
"It's very upsetting," he said. "They pay themselves
thousands of dollars."
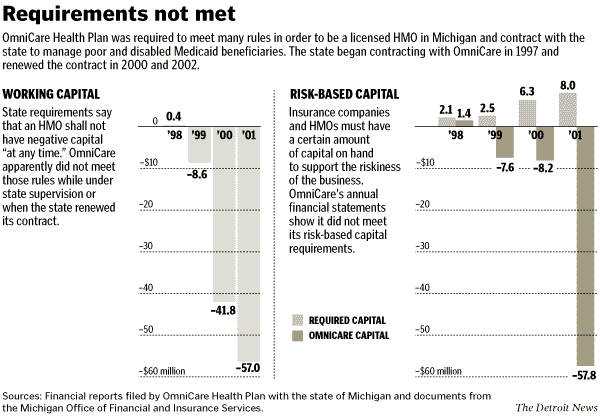
Auditors have refused to endorse OmniCare's annual financial
statements since 1998, saying the company would not turn over
required information. "We are unable to express an opinion on
the accompanying financial statements," KPMG of Detroit has
concluded year after year.
Despite this, State Insurance Commissioner Fitzgerald said
the audit was sufficient to meet the state HMO licensing
requirement that it have a certified financial statement.
OmniCare was losing as much as $2 million a month between
1999 and 2001, and doctors and hospitals that racked up millions
of dollars in unpaid bills are furious that the state did not
promptly fix the problems.
Fitzgerald asked Giddings in July 2001 to place OmniCare in
rehabilitation, a legal status that gives the state management
control of the company. When it first took over, the state
controlled all the assets of the company but did not make
operational decisions.
"Why did it take three years?" asked Dr. Dorothy Kahkonen,
president of the Michigan State Medical Society, which
represents 14,000 doctors statewide.
OmniCare's debt topped $100 million around July 2001, local
health care providers' records show. In the weeks before the
state filed for rehabilitation, OmniCare negotiated settlements
with creditors that reduced its liabilities to $64.5 million.
For example, negotiations reached with just the DMC and Henry
Ford Health System reduced that debt by $38 million.
Fitzgerald said he planned to file for the HMO's
rehabilitation in March 2001, when OmniCare filed its 2000
year-end financial statement, but the DMC was making movements
to purchase it. When the DMC backed off that deal, he said he
filed his request immediately.
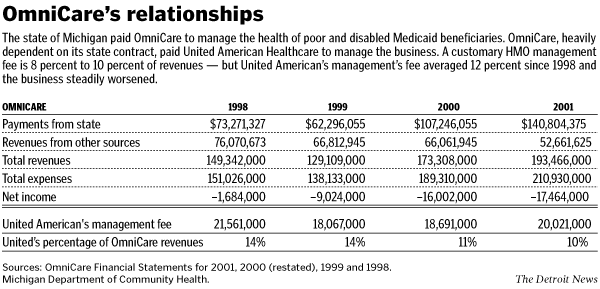
Failure won't occur
Insurance regulators are making an all-out effort to preserve
the health plan, citing OmniCare's important history in Detroit.
"Failure is not going to occur," Fitzgerald said.
But many hospitals and doctors are convinced the company
cannot be turned around because many patients and health care
providers may not want to do business with the company.
"We feel OmniCare is a grossly mismanaged, dishonest
organization that should no longer continue in business," Dr.
Leon Hochman, president of Southfield Obstetrical Services, said
in a letter to Giddings.
Dissatisfied Medicaid patients could opt out of the health
plan, jeopardizing its revenue, and it is unclear how many
doctors and hospitals the HMO would have in its network today if
Giddings hadn't ordered them to treat OmniCare patients.
William Beaumont Hospital officials said OmniCare will not
likely meet the contracting criteria for many health care
providers in the future. "There is a substantial likelihood
OmniCare will fail again," the hospital says in court filings.
Doctors and hospitals accuse the state of trying to revive
OmniCare in order to conceal problems with Gov. John Engler's
Medicaid program and avoid liability. Even if the multi-year
rehabilitation plan fails, the administration could avoid blame
through this fall's general election.
Before 1997, Medicaid patients could voluntarily enroll in
health plans but they were not required to do so.
Most patients remained in the traditional Medicaid program,
where they received services and the state simply paid their
bill. But the costs of that program were difficult to control
and were escalating rapidly.
So in 1997, Engler moved the state to a mandatory HMO program
for the poor and disabled, which allowed the services to be
performed for a fixed fee paid to health plans. The state was
able to trim $110 million from its annual $5.5 billion Medicaid
budget, but health care providers said that didn't leave enough
money to pay for the services.
Soon, doctors and hospitals bitterly complained they were not
getting paid on time, or at all, and they say the program has
been poorly managed. Many point to OmniCare as evidence of such,
and worry that other Medicaid HMOs will crumble as well.
Moses of United American said the state Medicaid department
is not paying HMOs enough to provide appropriate medical care
for patients.
Several health care companies have already laid off workers
and curtailed services in recent years because of losses caused
by OmniCare and other Medicaid HMOs. The DMC lost $66 million in
2001, and OmniCare was responsible for $55 million of that.
Health care providers insist the state of Michigan is
responsible for OmniCare's debts under federal law, which says
states are the "payer of last resort" under Medicaid. The state
of Michigan has denied any responsibility for the debts.
The financial situation was so bad at OmniCare in recent
years that it is questionable whether the state should have been
contracting with the company, some hospitals say.
When asked why the state was contracting with an insolvent
company, Fitzgerald said he was not responsible for Medicaid
contracts. Jim Haveman, director of the Michigan Department of
Community Health, which manages Medicaid, said he depended on
Fitzgerald's office to determine the financial soundness of
HMOs.
If the state had terminated its contract with OmniCare
earlier, it is unclear how the HMO could have emerged from the
red because more than 70 percent of OmniCare's revenues are
through Medicaid. That may have left the state on the hook for
the debts.
Fitzgerald, though, said he is trying to revive OmniCare for
other reasons.
"It has provided very good services to southeast Michigan,"
he said.

You can reach Sarah A. Webster at (313)222-1463 or
swebster@detnews.com.
|